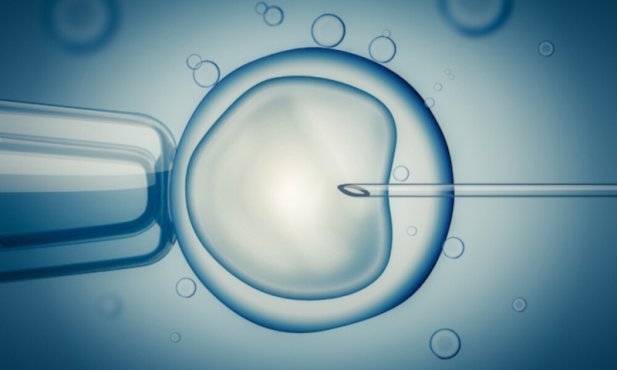
In vitro fertilization (IVF) has helped millions of people conceive, but it is not a single, uniform treatment. One important variation is intracytoplasmic sperm injection (ICSI), a technique in which a single sperm is directly injected into an egg. While standard IVF relies on sperm fertilizing the egg naturally in a laboratory dish, ICSI is used when fertilization is unlikely to occur on its own. Certain medical conditions make ICSI a more appropriate option than conventional IVF Treatment in Lahore.
One of the most common reasons for using ICSI is male factor infertility. This includes conditions such as low sperm count (oligospermia), poor sperm movement (asthenozoospermia), or abnormal sperm shape (teratozoospermia). When sperm are too few or too weak to penetrate the egg naturally, ICSI can bypass these barriers by placing a viable sperm directly inside the egg.
ICSI is also recommended for men with azoospermia, a condition in which no sperm are present in the ejaculate. In some cases, sperm can be surgically retrieved from the testes or epididymis using procedures like TESE or PESA. Because the number of retrieved sperm is often very limited, ICSI is required to achieve fertilization.
Another medical indication for ICSI is previous fertilization failure during standard IVF. If eggs fail to fertilize or show very low fertilization rates in a prior IVF cycle, clinicians may recommend ICSI in subsequent attempts to improve outcomes. This applies even when sperm parameters appear normal, as fertilization issues can sometimes be related to subtle sperm–egg interaction problems.
Certain genetic conditions also necessitate ICSI. For example, men with chromosomal abnormalities such as Y-chromosome microdeletions or those who have undergone vasectomy reversal may produce sperm that struggle to fertilize an egg naturally. ICSI allows fertilization while enabling careful genetic screening of embryos when indicated.
ICSI may be advised when using cryopreserved sperm or eggs, particularly if sperm quality declines after freezing and thawing. Similarly, eggs that have been frozen and later thawed can develop a hardened outer shell (zona pellucida), making it more difficult for sperm to penetrate without assistance.
In cases of unexplained infertility, ICSI fertility treatment is sometimes chosen after other treatments have failed. While not always medically necessary, it can reduce the risk of fertilization failure when the cause of infertility remains unclear despite thorough evaluation.
It is important to note that ICSI is not automatically better than standard IVF and is not recommended for all patients. When sperm quality and fertilization potential are normal, conventional IVF can be equally effective without the additional laboratory manipulation involved in ICSI.
Ultimately, the decision to use ICSI is based on individual medical findings rather than convenience or preference. A fertility specialist evaluates sperm parameters, reproductive history, and prior treatment outcomes to determine the most appropriate approach. Understanding the medical reasons behind ICSI helps patients make informed decisions about their fertility care.